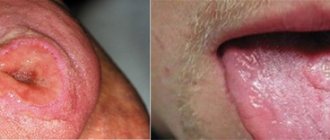
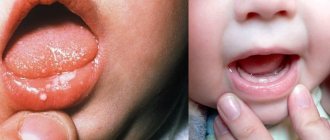
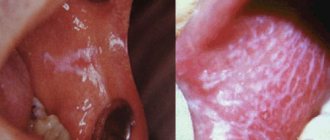
The oral mucosa is constantly exposed to some irritants. Even when eating food, the oral mucosa is affected by both mechanical factors (the very element of chewing food) and chemical factors: spicy and salty foods, hot drinks, alcohol, smoking. However, with the significant strength of local and general immunity, these effects do not cause significant harm to the mucous membrane, since the mucous membrane has good protective and regenerative properties. In this article we will look at traumatic lesions of the oral mucosa.
The protective mechanisms of the oral mucosa are specific, that is, immune defense, and nonspecific. Nonspecific protective factors include saliva and its components, such as lysozyme, dextrans, proteases and glycolytic enzymes, phagocytic factors, and complement factors.
All of the above protective factors of the oral mucosa do not always cope with their task, and when exposed to external (exogenous) factors, traumatic lesions of the oral mucosa occur.
Classification of traumatic lesions of the oral mucosa
The classification of traumatic lesions of the oral mucosa includes the course of injury, that is, traumatic lesions of the oral mucosa are:
- Acute traumatic injury to the oral mucosa;
- Chronic traumatic damage to the oral mucosa;
By their nature, traumatic lesions of the oral mucosa are divided into:
- Mechanical damage to the oral mucosa;
- Physical (radiation and thermal) damage to the oral mucosa;
- Chemical damage to the oral mucosa;
It is possible to distinguish a classification of traumatic lesions of the oral mucosa according to the factor that had a pathological effect:
- Home injury (domestic);
- Sports;
- Road;
- Production;
In principle, it is not so difficult to determine the nature of the injury, its course and the nature of its occurrence by carefully collecting an anamnesis.
Mechanical injury to the oral mucosa
Mechanical injury to the oral mucosa can be either acute or chronic. Determining the course of a mechanical injury to the oral cavity is not difficult; you just need to clarify the time of occurrence of the resulting mechanical injury.
Mechanical injury to the oral mucosa is one of the most common injuries, especially among men and children, meaning acute mechanical injury to the oral mucosa.
Etiology of acute mechanical trauma of the oral mucosa
The leading causes of acute mechanical injury to the oral mucosa are considered to be:
- Strikes. Impacts can be with a fist or an object, or against an object, for example, a fall.
- Bites;
- Injuries from cutting and piercing objects.
Clinic of acute mechanical trauma of the oral mucosa
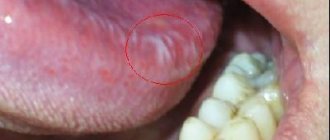
The clinical picture of acute mechanical injury is accompanied by slight pain. At the site of an acute mechanical injury there may be either erosion, an ulcer, or an area of hemorrhage. Often erosion and ulcers are irregular in shape, with unclear edges of the wound. Erosion on the oral mucosa heals quickly, but with secondary infection the erosion turns into an ulcer. If there was a hemorrhage, then after 1-3 days the color will change to bluish-purple or black-violet.
Treatment of acute mechanical trauma of the oral mucosa
Treatment of acute mechanical trauma to the oral mucosa does not present any difficulties. So, if there is bleeding, use hydrogen peroxide 1.5%; Treat the damaged area with a warm antiseptic solution; if there is significant pain, you can use an anesthetic, for example, 2% lidocaine. The patient is prescribed oral baths with a warm antiseptic solution and applications of foam aerosols (pentanol, hyposol). If the wound was very deep, then stitches should be applied.
Results and discussion
A study of the prevalence of TS showed that most often TS occurs in the first 1.5 months from the start of orthodontic treatment ( p
≤0.01), and subsequently the frequency decreases (Fig. 3).
Rice. 3. The incidence of traumatic stomatitis during orthodontic treatment in children and adults at various times during the active treatment period. Thus, according to the data we obtained, the incidence of TS was significantly less common than according to the literature [3–5], and amounted to 6.62–15.38% in children during different periods of the active period of orthodontic treatment with fixed appliances, and 4.69% in adults. -11.63% (see Fig. 2)
.
Before the start of treatment, TS of moderate and severe severity was detected in both children and young adults (Fig. 4, 5).
Rice. 4. The number of patients in the 1st and 2nd study groups depending on the severity of TS at different follow-up periods.
Rice. 5. The number of patients in the ٣-th and ٤-th study groups depending on the severity of traumatic stomatitis at different periods of follow-up. As a rule, the pain syndrome was mild, and the mucous membrane of the cheeks was most often affected, and less often the lips. Typically, in patients, regardless of age, with severe swelling and hyperemia, erosive and ulcerative lesions of varying severity were observed in the area of projection of orthodontic equipment (braces and arches).
The use of topical agents to treat TS has been effective in both children and adults. More pronounced positive dynamics of the reparative process of oral mucosa was noted when using gum gel with propolis in all age groups ( p
≤0.05) and observation period (
p
≤0.05).
At the same time, it should be noted that if in children on the 3rd day from the start of treatment TS of severe severity remained (see Fig. 4), then in young people (see Fig. 5) there was no such degree of TS ( p
≤0.05).
By this time, in adults, regardless of the drug used for the treatment of TS, there were no pathological changes in the mucous membrane in the area of the mucous membrane previously injured by the brace system ( p
≥0.05).
In children of groups 1 and 2, the effectiveness of treatment on the 3rd day was 34.66 and 48.96%, respectively ( p
≤0.01);
on the 5th day - 78.66 and 83.33%, respectively ( p
≤0.05). Similar data on the effectiveness of treatment of TS caused by injury to the mucous membrane of the cheeks and lips by braces and arches were obtained in young adults (Fig. 6).
Rice. 6. The effectiveness of treatment of traumatic stomatitis in patients of different groups at different periods of dynamic observation. Thus, in individuals included in the 3rd and 4th study groups, the effectiveness of treatment on the 3rd day was 60.29 and 68.03%, respectively ( p
≤0.05);
on the 5th day 91.18 and 95.08%, respectively ( p
≤0.05), which also indicated the greater therapeutic effectiveness of the gum gel with propolis for the treatment of TS caused by wearing fixed orthodontic appliances.
On the 10th day, no TS was detected in patients of all four study groups.
Chronic injury to the oral mucosa
Chronic injury to the oral mucosa involves exposure to an irritating factor for a long time. The main reasons for the occurrence of chronic trauma to the oral mucosa are:
- Overhanging edges of fillings;
- Unrestored contact point;
- Poor quality prostheses;
- Dental anomalies (teeth outside the dental arch, deep, open, cross bite);
- Metal ligatures;
- Poor quality tires;
- Bad habits.
All these factors trigger the catarrhal reaction. The severity of the inflammatory phases (exudation and proliferation) in these cases depends on the location of the stimulus, its strength and duration of action. Thus, some chronic mechanical injuries of the oral mucosa can be accompanied by serous, serous-purulent and purulent discharge. With purulent exudation, erosion occurs on the mucous membrane of the oral cavity, and as I wrote above: in the absence of treatment for erosion, an ulcer appears on the mucous membrane of the oral cavity; with mechanical trauma, it is called decubital (i.e., traumatic).
Clinic for chronic mechanical trauma of the oral mucosa
The clinical picture of chronic mechanical trauma to the oral mucosa is not characterized by a clear picture. Patients most often do not make any complaints. Complaints from chronic mechanical trauma to the oral mucosa are most often a feeling of awkwardness, discomfort, yes, there may be complaints of swelling and pain.
Erosion due to chronic mechanical trauma of the oral mucosa is not characterized by severe pain, which cannot be said about decubital ulcers. Decubital ulcers are very painful when eating and talking. If you examine it, the doctor may notice uneven edges, hyperemia along the periphery, fibrinous plaque in the center, which, when removed, reveals a bleeding surface. With the long-term existence of the ulcer, its edges become denser, rarely, but capable of epithelialization. Decubital ulcers can be of different depths; in the clinic, there have been cases when the depth of a decubital ulcer in chronic trauma of the oral mucosa reached the muscle layer.
Treatment of chronic mechanical trauma of the oral mucosa
First, treatment of chronic mechanical trauma to the oral mucosa should be aimed at eliminating the irritating factor. That is, all the fillings have been restored, the dentures have been adjusted (in principle, it is not recommended to wear dentures during the treatment of ulcers), and so on.
If it is painful, the erosion/ulcer should be treated with a warm anesthetic solution, the same 2% lidocaine. To facilitate the removal of necrotic or fibrin films, it is necessary to treat the wound with proteolytic enzymes for 1-2 minutes before starting this procedure. Foam aerosols, healing ointments such as solcoseryl, and keratoplastics (sea buckthorn and rosehip oil) are applied.
Symptoms and their manifestation
Symptoms characteristic of diseases in this category, in most cases, allow one to independently diagnose the presence of deviations from the norm. Notable changes include:
- The occurrence of itching and burning.
- The appearance of pain syndrome.
- Formation of tissue edema.
- Formation of ulcers and ulcers.
- Bleeding gums.
- Violation of the enamel structure.
- Constant unpleasant odor.
- Feeling weak and tired.
At the first signs of a pathological condition, it is recommended to seek help from specialists. Thus, in Dentika dental clinics you can undergo comprehensive diagnostics, which guarantees the accuracy of the diagnosis and the timely initiation of therapeutic measures.
Thermal damage to the oral mucosa
Thermal damage to the oral mucosa understandably occurs when exposed to excessive temperature. For example, hot food, drinks, careless work with a coagulator, incorrect electrophoresis technique. The degree of damage to the mucous membrane depends on the duration of the temperature stimulus. Therefore, a wound that occurs due to thermal damage to the oral mucosa can be:
- Limited;
- Spilled;
- Hyperemic;
- Blistered;
- With secondary infection;
- No secondary infection.
Clinic for thermal damage to the oral mucosa
The clinical picture of thermal damage to the oral mucosa is characterized by constant pain, aggravated by eating, talking, and any impact on the affected area. Often, with thermal damage to the oral mucosa, blisters appear, after opening which erosions occur. In more severe cases, a dark gray or black area of necrosis may occur.
Treatment of thermal damage to the oral mucosa
Treatment of thermal damage to the oral mucosa consists of the application of painkillers (for example, 2% lidocaine), treatment with low-concentration antiseptic ointments, and the use of foam aerosols. If erosion does not heal for a long time, keratoplasty can be used.
Change in structure with fluid accumulation
With such lesions, the structure of the mucous tissue changes so that a cavity filled with liquid is formed inside.
Bubbles and bubbles. They are formed in the epithelial layer or under it, filled with serous or hemorrhagic contents, and can be grouped. The cavity is closed by a thin layer of epithelium, which can break through. Bubbles can group and break quickly. Bubbles form and last longer. Both types of lesions provoke the formation of healing ulcers on the surface of the mucous membranes. They arise due to damage by viruses, traumatic injuries, and disturbances in tissue nutrition.
Ulcers. They can form from blisters or on unchanged mucosa. The cavity is filled with purulent exudate (whitish, yellowish, greenish contents with a pungent odor). They can be deep or superficial, often painful. Indicate an inflammatory process, appear after traumatic damage to the mucous membrane, due to infectious, viral diseases.
Cysts. A formation with dense walls that form a cavity. It is filled with transparent contents (can become purulent, serous, bloody). Appear due to blockage of gland ducts on the mucous membranes or as a symptom of periodontal diseases.
Radiation damage to the oral mucosa
Radiation damage to the oral mucosa is often an occupational injury if radiation therapy is not followed. In any case, all radiation injuries are called radiomucositis.
Etiology of radiation damage to the oral mucosa
The etiology of radiation damage to the oral mucosa includes:
- Inadequate exposure to radioactive substances;
- Failure to comply with the techniques and rules of radiation therapy (radiography, gamma irradiation, radio irradiation)