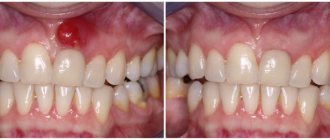
Periostitis of the jaw (flux) refers to dental diseases. The localization of the source of inflammation occurs in the periosteum. A subperiosteal abscess is formed, and the peri-maxillary soft tissues swell. A person experiences painful sensations radiating to the temporal region, ear, eye; his health worsens: weakness, sleep disturbances, fever, and headaches occur.
Periostitis, aka gumboil
The disease is diagnosed by inspection and palpation; an x-ray is required for confirmation. The doctor opens and drains the subperiosteal abscess and removes the tooth that is the source of infection. After this, the patient must undergo a course of physiotherapy and antibiotic treatment. It is also necessary to rinse your mouth regularly.
What kind of diagnosis is this? According to the international classification ICD-10, accepted throughout the world, periostitis of the lower jaw is assigned code K10.2.
Reasons for the development of periostitis
The causes of periostitis of the jaw are usually infection or injury. According to statistics, in practice this disease is observed in 5.4% of patients with inflammation in the face and jaw. Moreover, 95% of patients have an acute form, 5% have a chronic form. Localization of periostitis is observed one and a half to two times more often in the lower jaw. The clinical picture, both local and general, is peculiar. If the treatment process is started on time, it will end successfully, otherwise the disease progresses, which carries a high probability of severe purulent complications.
Why does this disease occur? There are several reasons. And the main one is complicated caries, in which pathogenic microflora penetrate through microchannels into the tooth cavity and then spread to the tissue surrounding the root.
Often periostitis is caused by chronic apical periodontitis. Diseased microorganisms move further and further through the channels over time. If the disease is not treated, the soft tissues are first affected, then the periosteum.
Staphylococcus always lives in the oral cavity. If the immune system is weakened, the population begins to grow and the periosteum becomes inflamed.
The hematogenous and lymphogenous form is usually caused by ENT diseases, ARVI, and infectious diseases such as measles and scarlet fever. Traumatic periostitis may occur after tooth extraction or trauma, surgical intervention, jaw fractures, infected wounds on the face, etc.
In many patients, periostitis is caused by previous hypothermia or overheating, as well as emotional or physical overload.
There are other reasons, less common: tuberculosis and other diseases that are fraught with complications spreading to the jaw periosteum.
The etiology and pathogenesis of periostitis in modern dentistry has been studied quite well. Treatment usually does not cause problems.
Periostitis of the jaw - symptoms and treatment
Treatment of periostitis is always surgical; if you deviate from this rule, there is a serious danger of a limited focus of inflammation flowing into a more dangerous - diffuse form, which will require different treatment tactics and often hospitalization of the patient.
Treatment of periostitis is standard and consists of eliminating the source of primary inflammation and evacuation of pus, i.e., removing the causative tooth (in cases of unfavorable treatment prognosis) and surgically opening the site to its entire width, followed by drainage.
The procedure is usually performed under local anesthesia; in some cases, drug sedation is indicated; anesthesia is also possible. You need to understand that the introduction of an anesthetic into tissues strained by exudate (fluid accumulation) is an extremely painful procedure, therefore, the method of pain relief before periostotomy (opening an abscess) has its own specifics: conduction anesthesia is preferable (a type of anesthesia when the nerve is blocked to the operation site) followed by local anesthesia performed superficially with a thin needle, without immersing the needle into the abscess.
The diseased tooth must be removed in the case of an unfavorable therapeutic prognosis: the presence of large foci of bone destruction, incorrect previously carried out treatment of the canals, resulting in their perforation or blockage by a fragment of an instrument, etc. In cases of a favorable prognosis, endodontic treatment is carried out, which involves the removal of pulp decay from the canals, appropriate mechanical and medicinal treatment of the canals with a special instrument and powerful antiseptics to eliminate infection in them, followed by temporary filling with calcium preparations and temporary filling of the tooth. Subsequent X-ray monitoring is very important in order to confirm the effect of the canal therapy: the focus of destruction in the bone should decrease and subsequently disappear.
To evacuate pus, periostotomy is performed (dissection of the mucosa and periosteum) along the entire length of the infiltrate along the transitional fold.
As a rule, the surgeon detects a characteristic symptom - detachment of the periosteum from the bone, whereas in a healthy state the periosteum is firmly attached to the cortex. At this stage, the abscess is emptied, or the absence of pus is detected along with the periosteal reaction. The surgeon uses a blunt instrument to probe the entire abscess cavity to identify isolated lesions. In the case of the presence of pus, irrigation (washing) of the subperiosteal space with antiseptics is usually carried out, followed by the introduction of drainage (usually a strip of glove rubber) into the wound to prevent its edges from sticking together. The wound is not sutured; the patient is given a dressing after a day or two to remove the drainage [8].
In the absence of contraindications, antibacterial therapy (in most cases, semisynthetic penicillins) and NSAIDs (nonsteroidal anti-inflammatory drugs) are prescribed. In case of severe edema, desensitizing drugs are prescribed. It is also necessary to prescribe analgesics or their direct intramuscular administration after surgery, since in the first hours after treatment, when the effect of the anesthetic wears off, severe pain symptoms appear. It also makes sense to locally cool the infiltrated area with ice for several hours to reduce bleeding and swelling. The cooling time must be assigned based on the patient’s subjective feelings, and not on specific time periods.
Almost always, this treatment leads to a positive result: within a few hours the patient experiences relief, decreased pain and swelling. Although the infiltrate in the form of a moderately painful compaction will persist for several days.
A follow-up visit the next day is necessary to confirm the results of the treatment and possible removal of the drain if there is no discharge from the wound. Subsequently, the patient is observed by a doctor for 3-5 days; it is quite legal to issue a certificate of incapacity for work for this period. After the pronounced symptoms of inflammation disappear, they begin to continue treatment of the causative tooth.
In rare cases, for example, when the incision is of insufficient length or when the drainage falls out and the edges of the wound stick together, treatment may be complicated due to a delay in the evacuation of residual pus from the lesion. In these cases, the incision should be widened and drainage should be ensured by introducing drainage.
Types and stages of disease development
The classification of odontogenic periostitis depends on the phase of the disease and the nature of its course. In addition to examination and palpation, the dentist prescribes an X-ray examination. The resulting image allows you to assess the condition of the roots and periapical areas. The image does not show thickening of the periosteum in the first three days from the onset of the disease.
- Various types of periostitis are classified according to the international classification ICD 10 depending on the route of infection into the periosteal tissue:
- acute odontogenic periostitis of the jaws (cause - diseased tooth);
- hematogenous (infection enters through the blood);
- lymphogenous (spread through the lymph system);
- traumatic (for injuries of the periosteum).
According to the course and pathomorphology, the disease is divided into two forms: acute and chronic.
In the acute form, the symptoms are pronounced. There is swelling of half the face, he is tormented by severe throbbing pain, and pus forms. The acute serous form is characterized by such clinical manifestations as infiltration in the periosteum, serous exudate is formed in the lesion. In acute purulent periostitis of the jaw (popularly called gumboil), a limited subperiosteal focus of inflammation is formed, fistulous tracts are formed, and pus comes out through them. The course of purulent periostitis is much more severe, with bursting pain that increases when drinking hot foods. If a fistula tract does not form, the dentist cuts the periosteum to allow the pus to escape.
The course of the chronic process is sluggish, stages of exacerbation occur periodically. Young bone tissue begins to grow on the surface of the jaw. With the development of the ossifying form, ossification and hyperostosis occur quite quickly. There are two degrees of spread of this process: limited (covering one to three teeth) and diffuse purulent (almost the entire jaw is covered).
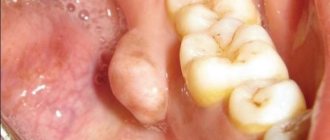
If the wisdom tooth erupts with difficulty, retromolar periostitis may develop in the lower jaw. The pus does not come out on its own due to anatomical features, which requires dissection.
Features of the treatment of dental periostitis
To treat tooth flux, conservative and surgical methods are used. The choice of treatment method depends on the causes and degree of neglect of the disease.
The conservative method (without surgery) is used:
- at the initial stage;
- caused by weak immunity;
- due to other inflammations in the body.
For non-surgical treatment of flux, anti-inflammatory and antibacterial drugs and physiotherapy are used. The tooth is not removed, but the gum is cut in the area of swelling and drainage is installed.
In the case of purulent inflammation associated with dental diseases (odontogenic periostitis), or when conservative treatment is ineffective, surgical intervention is used.
Characteristic symptoms
Symptoms of acute periostitis of the jaw are determined by the form of the disease. The state of the patient’s immune system and the diseases he has are also influenced. But there are also characteristic signs that make it possible to make an accurate diagnosis.
The disease develops gradually. At first, the gums swell a little, and pressing on the tooth causes pain. Having discovered such signs, the patient should visit a doctor on the same day, otherwise the cheek may become swollen by the morning.
Signs of the form of the disease with serous infiltrate are:
- red color of the mucous membrane:
- the appearance of painful swelling in the fold between the gum and cheek;
- tolerable pain;
- temperature may rise to 37°C;
- facial asymmetry;
- submandibular and postauricular lymph nodes enlarge (lymphadenitis).
With a purulent infection, the condition becomes much worse:
- signs of intoxication and pain are observed;
- temperature (up to 38°C);
- the cheek becomes swollen;
- pain radiates along the trigeminal nerve;
- pulsation is felt in the swollen part;
- a fistula may occur;
- When you press in the area between the cheek and gum, you can feel the vibrations of the fluid.
Causes and symptoms of periostitis
Symptoms of periostitis include swelling of the gums and face, suppuration, fever, and severe pain. The severity of dental flux manifestations depends on the form and severity of the disease. Swelling and asymmetry of facial contours depend on the location of the inflammation. With periostitis of the upper jaw, swelling of the upper lip, cheek and infraorbital area occurs. With periostitis of the lower jaw, swelling can be observed in the lower part of the face.
The causes of flux can be:
- failure to comply with hygiene rules;
- diseased or untreated teeth;
- consequences of complex tooth extraction;
- jaw injuries;
- infectious and inflammatory processes in the body;
- weakened immunity.
How is periostitis diagnosed?
For an accurate diagnosis, the doctor collects anamnesis, conducts an external and internal examination, prescribes an x-ray and examines the x-ray. Since the symptoms of some dental problems are identical, the surgeon must have a good understanding of their symptoms.
When conducting diagnostics, doctors look for similarities and differences between chronic periostitis of the jaw or acute and other diseases of the oral cavity. An x-ray helps differentiate the disease from others (apical periodontitis, phlegmon, abscess, inflammation of the salivary gland, osteomyelitis).
Apical periodontitis is characterized by the presence of a purulent focus located at the top of the root.
Cellulitis and abscess are manifested by external changes on the skin. An infiltrate appears on the affected area, the skin over it turns red and becomes shiny.
With sialadenitis, it is necessary to palpate the salivary gland to determine its density. Osteomyelitis is diagnosed by X-ray - in the early stage of the disease, it shows decaying bones, in the late stage - formed sequesters.
Stages of the operation
When treating periostitis of the jaw, the surgeon must cleanse the cavity of pus so that the process does not spread deeper. To do this, he cuts the periosteum. The operation consists of several stages:
- Anesthesia . The affected area is numbed using modern drugs.
- Periostotomy . The surgeon makes a soft tissue incision along the fold between the gum and cheek, capturing the periosteum. This ensures the release of purulent exudate to improve the patient’s condition.
- Wound drainage . A rubber or gauze graduate is installed into the incision. This ensures the drainage of pus.
After opening the purulent lesion, the surgeon asks the patient to rinse his mouth with a disinfectant solution.
After this, chlorhexidine and similar solutions are used to wash the wound. Measures such as irrigation with dimexide with oxacillin and 15-minute applications of dimexide liniment are also effective.
After examining an x-ray of the tooth that caused periostitis, the doctor decides whether it can be preserved and treated in the future to eliminate the source of infection, or whether tooth extraction is necessary.
Surgical intervention
With serous inflammation, as a rule, conservative therapy is limited. Pulpitis or periodontitis is treated, the patient is prescribed a course of physiotherapeutic sessions (UHF), rinsing with disinfectants. This leads to resorption of the infiltrate.
The acute purulent form requires surgical intervention to open the subperiosteal or submucosal abscess.
The milk tooth that caused periostitis must be removed. Severely damaged permanent teeth are also removed. Teeth that are capable of performing their functions need to be treated.
Treatment of various types of periostitis
Treatment of serous periostitis
Serous periostitis can occur due to jaw trauma. No special therapy is required to treat serous periostitis. At this stage, it is possible to clean the dental canal and create the opportunity for the independent release of fluid (exudate) during inflammation.
Treatment of acute purulent periostitis
In the case of acute purulent periostitis, the dentist cuts the gum, removes the pus and drains the suppuration. When draining, the tip of a rubber strip (drainage) is inserted into the cavity at the incision site. Drainage prevents the wound from healing too quickly and allows fluid to drain out. It is advisable to remove a diseased tooth, the source of infection of acute periostitis, if:
- severely damaged crown;
- obstruction of root canals;
- lost functionality;
- ineffectiveness of the non-surgical method;
- mobility.
In other cases, it is recommended to eliminate the relevant causes of infection (for example, inflammation of the tonsils and throat), as well as restore the immune system. The most effective approach to the treatment of acute purulent periostitis is complex therapy, combining surgery, drug therapy and physical therapy.
Treatment of diffuse periostitis
Diffuse periostitis is characterized by widespread infection, not limited to a local focus. This is a severe type of disease. As a rule, the patient needs the help of maxillofacial surgeons. In stationary conditions, an operation is performed to remove part of the periosteum or bone. Treatment of diffuse periostitis is complemented by drug therapy and detoxification.
Treatment of chronic periostitis
Chronic periostitis is a sluggish infection typical of patients with impaired immunity. If disease is present, the inflamed area is cleaned and physical therapy is prescribed to reduce symptoms and eliminate infection. In particularly difficult cases, the treatment of chronic periostitis may require serious surgical intervention to completely remove diseased tissue. In addition, with this form of flux, it is important to carry out therapy with vitamins and means to strengthen the immune system. An integrated approach stimulates an increase in the body's immunity.
Drug treatment
The second stage of treatment after surgery is drug therapy. The patient is washed with modern antiseptic compounds (Chlorhexidine, Ethacridine, Dimexide with Oxacillin), and sterile bandages are applied. To impregnate them, use a disinfectant solution or ointment. Antibiotics (Oletetrin, Oxacillin, Lincomycin) must be prescribed to prevent complications and relapses. Nitrofurans (Furadonin), sulfonamides, painkillers, antihistamines (Suprastin) may be prescribed; vitamins. In the period after the operation, the patient must follow a gentle diet and rinse with antiseptics.
Physiotherapy
After surgery, the patient is recommended to undergo a course of physiotherapy to stop the inflammatory process, solux lamp, ultrasound. These are procedures such as: UHF, fluctuarization, microwave, laser, electrophoresis. Usually 5 to 7 sessions are prescribed.
Is it possible to do without it? Such a serious disease as periostitis of the jaw cannot be cured at home; qualified professional help is needed from a professional who will eliminate the source of infection. You can use folk remedies only in cases where the pain comes on suddenly, and you need to somehow improve the patient’s condition. But you need to visit a doctor as soon as possible. Before this, you can rinse your mouth with soda, salt, a decoction of herbs that have an anti-inflammatory effect, apply cold compresses to reduce swelling and relieve pain.
Treatment of gumboil with folk remedies
In order not to harm the body, folk remedies for treating flux can only be used for temporary pain relief or as a supplement during the recovery period.
- Infusions of oak bark, sage, St. John's wort, and calendula are used to rinse the mouth (strictly warm solutions).
- Chamomile flower tea is taken orally and is also used as a mouth rinse.
- Honey or honey propolis products are used to lubricate the gums.
In case of treating periostitis at home, you should consult a doctor. In any case, you should not postpone a surgical visit to the dentist when the first symptoms of gumboil appear on the gums or replace medical therapy with self-medication. When treating flux only with folk remedies, inflammation can spread further or develop into chronic periostitis.
With a timely and comprehensive approach to the treatment of periostitis, the disease is successfully cured. However, full recovery will require the help of a qualified dentist, medical procedures and medications.
What to do for prevention
The main preventive measure is to constantly monitor the condition of the oral cavity. Preventive measures include:
- daily hygiene of teeth and gums;
- visiting the dentist twice a year;
- use of professional hygiene procedures, removal of tartar;
- timely treatment of caries and other pathologies;
- If you have problem gums, you need to be systematically treated by a periodontist.
To prevent periosteal disease, doctors recommend having an x-ray every year.
Periostitis of the jaw often develops even in children.
If you notice swelling on the face of a child complaining of pain, immediately take him to the dental clinic. Self-medication is unacceptable! Taking some medications may disrupt the picture of the disease, which will complicate the diagnosis and may result in serious complications. Moscow metro station Zvezdnaya, Danube Avenue, 23