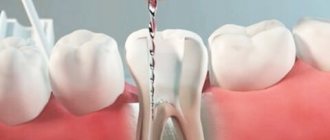
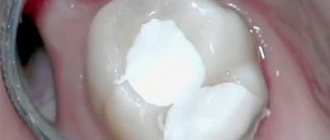
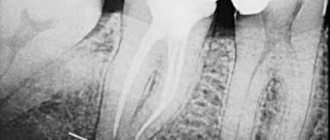
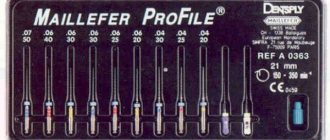
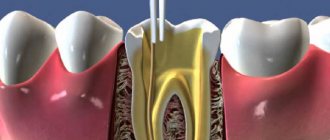
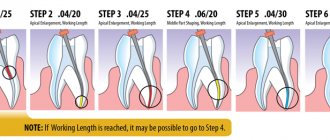
The working length of the root canal is the distance from the end point at the apex to the external landmark chosen by the doctor (tubercle, filling on the coronal part).
Doctors still cannot come to a consensus and say what should be taken as a guide: the physiological foramen (the transition of root cement into dentin), the apical foramen (the hole itself), the radiographic apex (the most distant point on the image) or the anatomical apex (the most distant area from the crown). The distance between them is up to 2 mm, and this is the difference between a well-sealed canal and the preservation of a source of infection.
The most important task is to find this end point, which is complicated due to the large number of different anatomical structures.
There are 4 methods for determining the working length of the root canal:
- x-ray
- tactile
- using an apex locator
- tabular
X-ray
The doctor determines the radiological apex from the image and the working length of the root canal is set 1 mm before it. The problem is that the channel is a three-dimensional structure, and the image is presented to us in a two-dimensional projection. There are cases when the doctor perforated the canal wall, while on the x-ray everything looks within normal limits. In almost 50% of all cases, the instrument is deeper than it appears in the photo.
Features of determining the working length of temporary teeth
If it is necessary to measure canals at the stage of active root formation in young patients, the specialist needs to take into account some nuances. For example, in this case, the X-ray method will be the most accurate. In this case, keeping the rudiments of permanent teeth intact is of great importance. For this purpose, doctors and dentists are advised to adhere to the following recommendations:
- Instrumental treatment of primary teeth should be carried out at a greater distance from the extreme radiographic line than in the case of treatment of permanent teeth.
- Even if there are signs of root resorption on the images, the size of the endodontic instruments should be 2-3 mm shorter than the radiographic length of the tooth.
- When processing canals, it is important not to reach the boundary line of about 2 mm, which will preserve the integrity of the root growth zone.
The correct choice of treatment method and competent calculation of the length of dental canals in children of different ages is a key factor in successful therapy and prevention of complications.
Tactile method
The least reliable option for determining the length of the root canal, the quality of such diagnostics depends on the doctor’s “insight” and his experience, which, you see, is an unacceptable argument. A thin instrument is inserted into the canal and the location of the hole is determined by touch. Another method is to use a paper point. Where it is saturated with blood or other contents is considered the exit point. If not a small part, but a significant area is saturated with blood, then it should be concluded that it has gone beyond the apex. This can also include pain. When the instrument goes beyond the top, the patient feels a prick, which is what the doctor focuses on.
Computed tomography in endodontics: a model of modern treatment
Radiography is an important aspect of successful diagnosis of odontogenic and non-odontogenic pathology, treatment of the pulp chamber and root canals through coronal access, biomechanical treatment of root canals, final canal obturation and evaluation of the treatment performed. Images are required throughout the endodontic treatment. Obtaining an image before the intervention is required for a correct assessment of the hard tissues of the tooth and alveolar process, as well as the degree of pathological damage and making the correct diagnosis. Further, obtaining images throughout the treatment is also necessary. Taking an image at the end of treatment allows you to evaluate the manipulations performed. Kells first reported the use of a conductive conductor in the root canal in a "radiograph" in 1899.
Since then, radiology has always played a key role in endodontics. Now, a century later, early efforts have led to the invention of computed tomography (CT) and micro-CT, and the introduction in 1996 of cone beam computed tomography (CBCT) provided the 3D images needed in dental practice.
This new 3D imaging capability has significantly improved the standard of dental treatment around the world. CBCT is gradually becoming the gold standard in providing accurate diagnosis, treatment planning and treatment. Cone beam technology currently has many applications in dentistry, including implant planning, surgical pathology assessment, TMJ assessment, growth and development detection for orthodontic purposes, pre-operative, operative and post-operative assessment for craniofacial trauma, craniofacial reconstruction and oral surgery. . In addition, CBCT is used to identify the exact location of the foreign body in the soft tissue, identifying cleft lip and palate, and the depth of the carious lesion. CBCT is becoming a typical tool in the work of a surgeon, especially an implantologist.
Limitations of 2D Images
The image obtained with a conventional radiograph is a two-dimensional (2D) interpretation of a three-dimensional (3D) object. Characteristics of a 3D object, such as complex dental anatomy and surrounding tissue structure, may be difficult to discern as “shadows” in a 2D image, which can lead to inappropriate endodontic treatment. When analyzing a 2D image, all images are interpreted very freely, introducing an aspect of subjectivity. Limitations of dental radiography may also be due to radiologist error. Any inaccuracies in image acquisition, ranging from incorrect angulation to incorrect configuration of the tooth in relation to the sensor, can lead to errors in the interpretation of the images. Such images of poor quality have artifacts and contribute to incorrect diagnosis. Many researchers, including Goldman, have confirmed the low correlation (47%) among all specialists treating periapical pathology using dental radiography.
Cone beam computed tomography
CBCT has been used in dentistry since 1981. Unlike a regular CT scan, which creates an image in different layers, CBCT creates an image in 3D pixels called voxels. Since these voxels are isotropic, the object is carefully measured in different directions. This allows you to visualize a geometrically undistorted image of the maxillofacial area, which can be viewed from different angles. In addition, to provide high image resolution, CBCT is available for viewing from different viewpoints (FOV) for use in a variety of situations. In endodontics, an apparatus with a limited FOV is usually sufficient. Typically, the smaller the scan volume, the higher the spatial resolution of the image. Since an early symptom of periapical pathology is discontinuity of the lamina dura and widening of the periodontal fissure, the optimal resolution for CBCT imaging used in endodontics should not exceed 200 nm - the average width of the periodontal space. 3D Accuitomo (K Morita, Corporation, Kyoto, Japan) - the first of the small FOV systems - provides a resolution of 0.125 mm. Orthophos XG3D (Sirons Germany) also provides a 5*5 FOV specifically for endodontic purposes.
CBCT produces much less radiation exposure than conventional CT. The exposure dose when performing digital radiography is comparable to taking conventional diagnostic panoramic or targeted images. Acquiring images for the entire mouth is irradiated at approximately 150 usv. It is obvious that a high-resolution CBCT scan of one tooth, used in the diagnostic process, replaces 3 targeted images. It is difficult to imagine that exposure dose could be more important than obtaining CBCT in a prudent manner to obtain information that is simply not available with other instruments.
CBCT in endodontics
1. Assessment of root canal morphology
The success of endodontic treatment depends on locating all root canals and then evaluating, cleaning, debridement and obturation. The frequency of occurrence of the second mesiobuccal canal (MB2) in maxillary first molars varies from 69% to 93% depending on the chosen method of examination. This variability occurs in the buccolingual plane, where overlapping anatomical structures prevent the identification of structures with small differences in shadow density. Conventional radiography, at best, can only detect 55% of these configurations.
Ramamurthy and Matherene describe the limitations of 2D imaging for identifying MB2 channels (Figure 1).
Photo 1: MB2 image in both first molars
A study conducted by Neelkantan in Indian population found that MB2 canal is most common in the first maxillary molar compared to the second. Also, anatomical type IV canal is more common than in the Mongoloid population.
Baratto Filho examined the internal morphology of extracted maxillary first molars, comparing them with microscopic examination and ex vivo CBCT imaging. Reports showed the presence of 4 canals in 67.14% of teeth and additional root canals in 92.85% of cases in the mesiobuccal root. Clinical evaluation showed a slightly reduced overall rate (53.26%) but an increased detection rate of MB2 (95.63%), while CBCT showed 37.05%. The scientists concluded that CBCT is a good method for the initial assessment of the internal morphology of the upper first molar, but for identifying the orifices, the use of a microscope is the best method. CBCT has also been used to identify the high incidence of distolingual canal in Taiwanese, identify abnormalities in the root canal system of mandibular premolars, and help identify root deviation (Figure 2).
Figure 2: Axial view of C-shaped canals in second molars
With the invention of the new CBCT software Orthophps CG3D/Galelios (Sirona, Germany), the working length of the canals also became feasible. But the accuracy of these data in clinical work has yet to be confirmed (Photo 3).
Photo 3: Tool for measuring the length of the root canal
2. Pathologies in periapical tissues
The most common pathological condition affecting teeth is inflammation of the pulp and periapical areas. CBCT technology now provides the clinician with the ability to view the desired area in three different planes, thereby obtaining 3D information. Lesions contained in cancellous bone with little or no cortical plate may be difficult to diagnose on plain film. Lofthag-Hansen, Stavropoulos, and Wenzel compared the accuracy of limited-FOV CBCT with conventional imaging.
The researchers reported that CBCT provided more accurate diagnostic data (61%) compared with digital (39%) and conventional (44%) radiographs. But although CBCT data is more accurate, researchers are not calling for the complete replacement of conventional intraoral radiography for detecting periapical changes in routine clinical practice due to financial and harmful components. Estrela et al proposed the use of CBCT-based periapical indices to identify pathologies (Figures 4-6).
Figure 4: Periapical cyst in the anterior segment of the mandible A: 3D view showing a large cystic cavity B: Sectional view showing loss of cortical plate C: Axial view showing loss of cortical plate on the labial side and intact plate on the lingual side.
Figure 5: Chronic periapical abscesses around the right mandibular first molar
Photo 6: Periodontal lesions near the upper left second molar
The CBCT index system consists of 6 grades (0-5) based on determining the largest lesion size in any dimension and taking into account the expansion and destruction of cortical bone.
Using this index, Low came to the conclusion that it is better to use CBCT weeks or conventional radiography to detect periapical pathologies.
Shadow gradient CBCT can help in the differential diagnosis of cyst and granuloma. In general, the ability to detect pathologies of CBCT is as good as that of plain CT. This method can be important for patients who present with pain or poorly localized complaints in the area of previously treated or untreated teeth, where pathology is not detected on a regular x-ray.
3. Root fractures
The usefulness and importance of CBCT in the diagnosis and management of dentoalveolar trauma, especially root fractures, luxation, displacement and alveolar bone fracture, have been extensively studied.
CBCT has found application specifically in the diagnosis of tooth root fractures.
(Photo 7,8) The high importance of CBCT in identifying vertical and horizontal root fractures has also been described in the literature. Elimination of superimposed anatomical structures allows the clinician to clearly analyze the fracture. In addition, 3D reconstruction can be performed on both the dentofacial system and the alveolar bone.
Figure 7: Root fracture in an endodontically treated upper right second molar A: OPG showing previously treated canals of an upper right first molar B: Axial image showing the fracture line along the palatal root C: Sectional view showing the oblique fracture line of the palatal root
Figure 8: Horizontal fracture of the right upper central molar A: 3D image showing the fracture line at the junction of the middle and apical third of the root B: Axial image showing the horizontal fracture line in the anterior aspect of the upper right central incisor C: Oblique fracture line extending from the mesial carp central incisor on a sectional photograph.
4. Root resorption
Root resorption is the loss of hard tooth tissue as a result of osteoclast activity. This may occur as part of a physiological or pathological process. Root resorption can be classified into external and internal, depending on the location of the process relative to the root surface. The first data on internal resorption were obtained in 1830. In comparison with external resorption, internal resorption is a very rare process, the etiology of which is not fully understood. The accuracy of CBCT in determining surface defects, although higher than that of standard techniques, is still not ideal and increases with increasing voxel resolution of the image. CBCT has also been shown to be useful in assessing post-orthodontic apical resorption, in particular the roots of the maxillary lateral incisors in impacted canines.
On CBCT, external resorption appears as uneven radiolucency and an intact tooth canal, while internal resorption appears as a clear focus without tracing the root canal.
CBCT has been successfully used to determine internal resorption and differentiate it from external resorption. Conventional radiography often cannot reveal the correct extent of distribution, localization and source of the resorptive process. CBCT helps in determining treatment tactics, and also offers an accurate prognosis based on the activity and extent of the lesion. Both the treatment and the treatment outcome become more predictable in this way.
5. Postoperative assessment
Monitoring the healing process of apical lesions is an important aspect in the postoperative phase of endodontics. Also, adequate root canal obturation is an important determinant of endodontic success. It can be stated that CBCT is very useful both in starting treatment and in monitoring the subsequent condition of the tooth. Sogur reports that images obtained from conventional X-rays in the postoperative period are more informative than CBCT. The scientist explains this fact by the presence of a large number of artifacts in CBCT images, caused by the presence of gutta-percha and sealer in the canals (Photo 9).
Photo 9: Artifacts of obstructed root canals
The use of CBCT in determining the exact location of the perforation and its role in the subsequent treatment plan is illustrated by Young (Figure 10).
Figure 10: Root perforation clearly visible on axial image
Preoperative assessment of periapical tissues is an important step to prevent complications. The close location of the apex to the mandibular canal, mental foramen and maxillary sinus can be assessed specifically on CBCT images. Rigolone was the first to describe the importance of CBCT for endodontic intervention planning.
The importance of CBCT for apical surgery of teeth close to the maxillary sinus was consistently demonstrated by Nakata, who demonstrated a clinical case of periradicular pathology localized to a specific root. Tsurumachi and Honda described the use of CBCT in locating an endodontic instrument fragment that had entered the maxillary sinus.
Conclusion
Despite the obvious advantages of CBCT technology in dentistry, there are also some disadvantages and limitations. CBCT technology is not currently widely available. Gradually, with the introduction and mastery of specialists, CBCT will become a more common diagnostic method. Although this technique has been on the market for several years, it continues to be expensive. For most endodontic procedures, only a small FOV of 4*4 mm is sufficient.
Limiting the FOV not only reduces radiation dose, scan time and artifacts, but also focuses on structures that are familiar to dentists. What is expected in the future regarding endodontics to CBCT? It is not known whether dentists will want to purchase the device themselves or receive images from a special radiologist from the center. One thing is clear: more and more dentists are introducing CBCT into their practices.
Author: Sushma Prashant Jaju , BDS, MDS Operative Dentistry and Endodontics, Dentocare multispecialty Dental Clinic, Nashik, Maharashtra, India
Apex locator
The electronic method is considered the most reliable of all mentioned. The most popular brands of devices are: Russian Geosoft (EndoEst), Japanese NSK (iPex), German VDW (Raypex).
Determination of the working length of the root canal:
- one wire with a hook at the end is hung on the patient’s lip
- diagnostic tool (for example, K-file) is installed in the holder
- then the doctor slowly moves it along the canal; numbers are displayed on the device screen indicating how much is left to the top. An intermittent beep will also sound. Some models have a graphic display: green - far, yellow - close, red - in place
- When the instrument reaches its destination, APEX will appear on the screen and the alarm will beep continuously.
Table method
Over a long period of clinical observations, doctors have accumulated an extensive database on the working length of root canals. So, if there are no other options, you can take a conventional cutter and check the readings in the table. If there is no apex locator and x-ray, then this method should be supplemented with tactile. However, the anatomy of each person is individual, so the reliability of the table values is also not high.
So what is the most effective method for determining the working length of a root canal?
Alas, there is no one ideal technique. At the moment, it is customary to rely on the “apex locator + x-ray” combination.